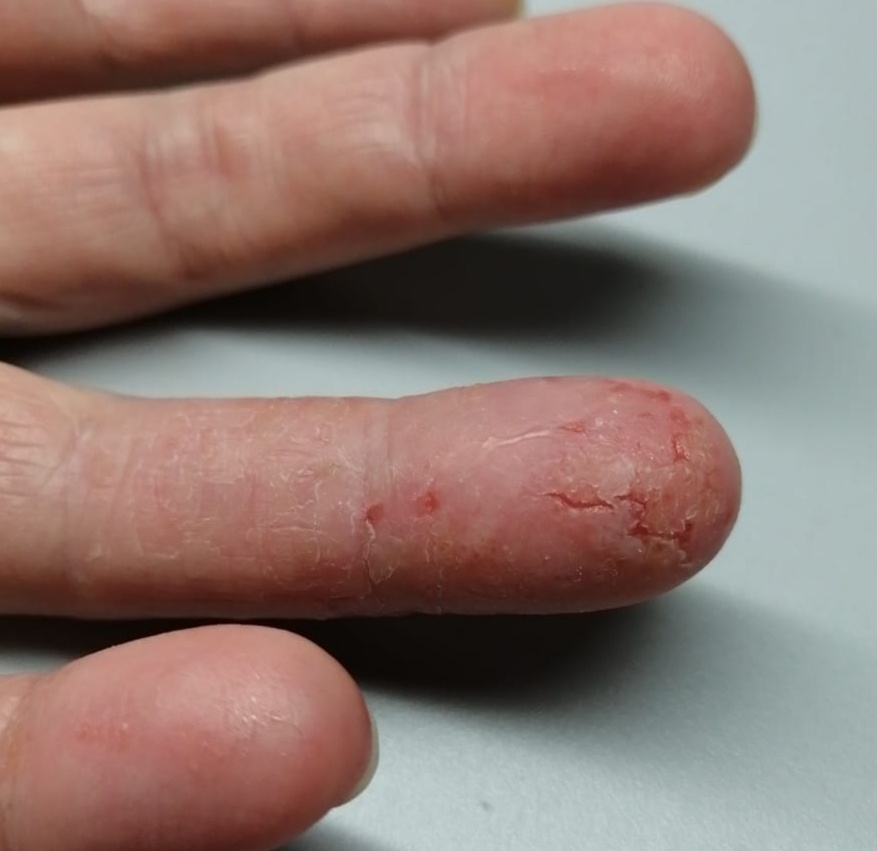
Eczema develops from a mix of genetic tendency, a weakened skin barrier, and an overreactive immune system, then is triggered by things like stress, irritants, infections, and other illnesses. Primary factors are your inherited skin and immune traits; secondary factors include stress, hormonal and gut issues, infections, and unsuitable skin or household products.
You’re more at risk of eczema if it runs in your family, you have allergies or asthma, very dry or oily skin, varicose veins, or chronic infections. Frequent contact with irritants, stress, sweating, and some internal diseases like endocrine or gut disorders also increase the chance of flares.
Eczema treatment combines anti-inflammatory medicines (usually topical steroids or calcineurin inhibitors), itch control, and gentle daily skin care with fragrance-free emollients. Just as important are finding and avoiding triggers, treating any infections or vein problems, following a hypoallergenic diet if advised, and using our AI skin analysis to monitor how your skin responds over time.
To prevent eczema flares, keep your skin well moisturized, avoid harsh soaps and irritants, and manage stress and sweating. Wear protective clothing or gloves at work if you handle chemicals, treat vein or circulation problems, and use our AI skin analysis to catch early changes before a full flare develops.
See a dermatologist to confirm the type of eczema, rule out infections or other skin diseases, and build a long-term treatment and skin-care plan. You should seek medical help sooner if the rash is very widespread, extremely itchy, infected, or not improving with basic moisturizers and over-the-counter creams.
Most eczema can be seen by a dermatologist on a routine basis, but you should seek earlier care if there is severe itching, widespread rash, signs of infection (pus, yellow crusts, fever), or painful leg eczema with swelling and varicose veins.